Table of Contents
Abstract
This paper explores the complex and paradoxical relationship between caffeine and migraine headaches. While caffeine is commonly used as an ingredient in migraine medications due to its pain-relieving properties, it can also trigger migraine attacks in susceptible individuals. Through a review of current literature, this paper investigates the mechanisms underlying this dual relationship, examining how caffeine interacts with adenosine receptors, affects cerebral blood vessels, and influences other biochemical pathways relevant to migraine pathophysiology. Understanding this complex relationship can help clinicians and patients better manage caffeine consumption to optimize migraine treatment and prevention.
Introduction
Migraines are a common and debilitating neurological disorder affecting approximately 12% of the population globally 1. Characterized by intense headaches, often accompanied by nausea, vomiting, and sensitivity to light and sound, migraines significantly impact quality of life. The pathophysiology of migraine is complex, involving neuronal dysfunction, inflammatory processes, and vascular changes 2.
Caffeine, a methylxanthine compound found in coffee, tea, chocolate, and various medications, is one of the most widely consumed psychoactive substances worldwide. Its relationship with migraine headaches is particularly intriguing due to its seemingly contradictory effects. On one hand, caffeine is a common ingredient in many over-the-counter headache remedies and can enhance the efficacy of analgesic medications. On the other hand, it can act as a migraine trigger for susceptible individuals and contribute to medication overuse headaches 3.
This paper aims to explore the potential mechanisms by which caffeine can both trigger and alleviate migraine symptoms, and to discuss strategies for managing caffeine intake in migraine patients. By understanding this "double-edged sword" relationship, healthcare providers can better guide patients in optimizing their caffeine consumption to manage migraine effectively.
Caffeine as a Migraine Trigger
For many individuals with migraine, caffeine can act as a trigger for attacks. Several mechanisms may explain this effect:
Caffeine Withdrawal
Regular caffeine consumption leads to physiological dependence through adaptations in the central nervous system, particularly involving adenosine receptors. When caffeine intake is abruptly reduced or stopped, withdrawal symptoms can occur, with headache being one of the most common manifestations 2. For migraine-prone individuals, these withdrawal headaches can evolve into full-blown migraine attacks.
Cerebral Blood Flow Changes
Chronic caffeine consumption leads to tolerance of its vasoconstrictive effects. Upon caffeine withdrawal, rebound vasodilation occurs, increasing cerebral blood flow. This hemodynamic change can potentially trigger a migraine attack in susceptible individuals 4. Furthermore, the fluctuations in cerebral blood flow associated with irregular caffeine consumption may contribute to migraine vulnerability.
Individual Sensitivity
Genetic factors may influence individual sensitivity to caffeine as a migraine trigger. Variations in genes encoding adenosine receptors, caffeine-metabolizing enzymes, and proteins involved in neurotransmitter regulation may explain why some migraine sufferers are particularly sensitive to caffeine's triggering effects 3.
Caffeine as a Migraine Reliever
Despite its potential to trigger migraines, caffeine is often used as an adjunct in pain relievers to treat acute migraine attacks. Several mechanisms contribute to its therapeutic efficacy:
Enhanced Analgesic Effects
Caffeine enhances the analgesic effects of medications like acetaminophen, aspirin, and ibuprofen. When combined with these analgesics, caffeine can increase their absorption and efficacy, providing more rapid and effective pain relief 5. This synergistic effect makes caffeine a valuable component in many migraine-specific medications.
Vasoconstrictive Properties
Caffeine acts as a vasoconstrictor, potentially counteracting the vasodilation that occurs during migraine attacks. By constricting dilated blood vessels in the brain, caffeine may help reduce cerebral blood flow and alleviate headache pain during a migraine episode 1. This effect is particularly beneficial for individuals who infrequently consume caffeine and have not developed tolerance to its vasoconstrictive properties.
Adenosine Receptor Antagonism
Caffeine blocks adenosine receptors, particularly the A1 and A2A subtypes, which are involved in pain perception. By inhibiting these receptors, caffeine can reduce pain signaling and provide relief during migraine attacks 2. This mechanism may contribute to caffeine's effectiveness as a migraine treatment, especially when used in combination with other analgesics.
Mechanisms of Action
Caffeine's complex effects on migraines are mediated through several molecular and physiological mechanisms:
Adenosine Receptor Antagonism
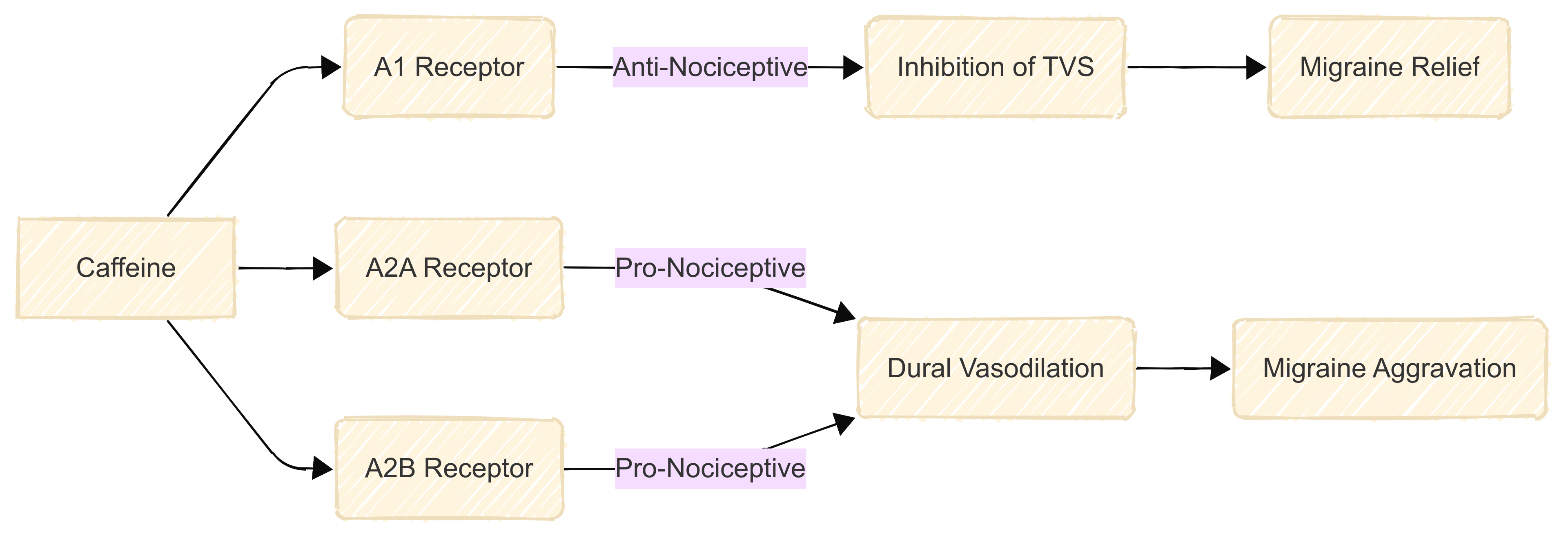
Caffeine is a competitive antagonist of adenosine receptors, primarily affecting A1, A2A, and A2B receptor subtypes 5. The blockade of these receptors has diverse effects depending on the receptor subtype and brain region. A1 receptor antagonism may produce anti-nociceptive effects by inhibiting the trigeminal vascular system, while A2A and A2B receptor antagonism can have pro-nociceptive effects through dural vasodilation. This differential effect on receptor subtypes may partially explain caffeine's dual role in migraine.
Fig.1. Caffeine's Interaction with Adenosine Receptors and Migraine Outcomes
Vasoconstriction
Caffeine's ability to constrict blood vessels in the brain can reduce cerebral blood flow, potentially alleviating headache pain. This vasoconstrictive effect is particularly relevant in migraines, where vasodilation is thought to play a role in the pathophysiology of the headache phase. Caffeine's vasoconstriction may also be related to inhibition of phosphodiesterase (PDE), leading to increased levels of cyclic adenosine monophosphate (cAMP) in vascular smooth muscle cells 2.
Neurotransmitter Regulation
Caffeine can influence the release and activity of various neurotransmitters, including dopamine, serotonin, and glutamate. These neurotransmitters play crucial roles in pain perception and migraine pathogenesis. For instance, caffeine's ability to enhance dopaminergic transmission may contribute to its analgesic properties, while its effects on serotonergic pathways could influence migraine susceptibility (Hoffmann et al., 2019).
Anti-inflammatory Properties
Some research suggests that caffeine possesses anti-inflammatory properties, which could be beneficial in migraines where neurogenic inflammation plays a role. By inhibiting inflammatory processes in the trigeminovascular system, caffeine may help reduce migraine pain and duration 2.
Magnesium Modulation
Caffeine consumption can affect magnesium levels, and magnesium deficiency has been implicated in migraine pathophysiology. Chronic caffeine intake may reduce magnesium availability, potentially exacerbating migraine susceptibility in some individuals 3. Conversely, acute caffeine consumption might temporarily increase magnesium utilization, which could contribute to its pain-relieving effects.
Clinical Implications and Management Strategies
Understanding the dual relationship between caffeine and migraines has important implications for clinical management:
Individualized Approach
Given the variable effects of caffeine on migraines, an individualized approach to caffeine management is essential. Some patients may benefit from moderate caffeine consumption, while others may need to avoid it entirely. Healthcare providers should help patients identify their personal caffeine threshold and develop appropriate consumption strategies 1.
Consistent Caffeine Intake
For migraine patients who regularly consume caffeine, maintaining consistent daily intake is crucial to prevent withdrawal headaches. Abrupt changes in caffeine consumption should be avoided, as they can trigger migraine attacks. If caffeine reduction is necessary, it should be done gradually to minimize withdrawal symptoms 4.
Monitoring and Tracking
Keeping a headache diary that includes caffeine consumption can help patients identify patterns and relationships between caffeine intake and migraine attacks. This information can be valuable for optimizing caffeine management strategies and improving overall migraine control 3.
Cautious Use in Acute Treatment
While caffeine can enhance the efficacy of acute migraine medications, its use should be monitored to prevent medication overuse headaches. Patients should be educated about the potential risks of frequent use of caffeine-containing analgesics and the importance of limiting their consumption to prevent the development of chronic migraines 2.
Conclusion
Caffeine's role in migraine is complex and individualized, representing a true "double-edged sword." It can be a valuable tool for relieving acute migraine pain for some individuals, while it can trigger attacks in others. This duality stems from caffeine's multiple mechanisms of action, including its effects on adenosine receptors, cerebral blood flow, neurotransmitter regulation, inflammation, and magnesium levels.
The impact of caffeine on migraines is influenced by various factors, including genetics, habitual consumption patterns, dosage, and individual sensitivity. This complexity necessitates a personalized approach to caffeine management in migraine patients, with strategies tailored to each individual's unique response.
Given the potential for both benefit and harm, careful tracking of caffeine consumption and its relationship to migraine occurrence is essential. Keeping a headache diary can help individuals identify their sensitivity threshold and optimize their caffeine intake accordingly. Consultation with healthcare providers is recommended to develop a tailored caffeine management strategy, which may include gradual adjustment of caffeine intake, identification of caffeine withdrawal symptoms, and suggestions for appropriate caffeine alternatives.
Future research should focus on exploring caffeine's impact on different migraine subtypes and their genetic influences, studying the interactions of caffeine with other migraine treatments to determine optimal dosing regimens, and further elucidating the molecular mechanisms by which caffeine affects migraine pathophysiology 2. A more comprehensive understanding of the relationship between caffeine and migraine will enable clinicians to provide more precise and effective management strategies for migraine patients, ultimately improving their quality of life.
References
Mayo Clinic Health System. (n.d.). Caffeine's effect on headaches. Retrieved from https://www.mayoclinichealthsystem.org/hometown-health/speaking-of-health/does-caffeine-treat-or-trigger-headaches↩
Zahedi, A., Ghorbani, Z., Haghighi, M., Zavareh, A. D., & Mohammadi, M. (2020). The ambiguous role of caffeine in migraine headache: A systematic review. Journal of Headache and Pain, 21(1), 1-11. https://doi.org/10.1186/s10194-020-01167-2↩
Hoffmann, J., Gaul, C., & Dlugaj, M. (2019). Caffeine and primary (migraine) headaches—Friend or foe? Frontiers in Neurology, 10, 1275. https://doi.org/10.3389/fneur.2019.01275↩
WebMD. (n.d.). Migraines and headaches: Triggers: Caffeine. Retrieved from https://www.webmd.com/migraines-headaches/triggers-caffeine↩
Ferré, S., Fredholm, B. B., Morelli, M., Popoli, P., & Fuxe, K. (1997). Adenosine receptor subtypes and their functions in the central nervous system. Journal of Pharmacology and Experimental Therapeutics, 282(2), 425-439.↩